Artificial cell tissue grown with embedded wiring opens way for 'cyborg' organisms
10 September 2012
A team from Harvard University and MIT has developed a method of growing artificial tissue on a 3D structure of microscopic electrical wires.
This is the first time that electronics and artificial tissue have been truly merged in 3D, allowing direct sensing and potentially stimulation of the tissue. It could lead to the development of engineered tissues that incorporate capabilities for monitoring and stimulation, and of devices for screening new drugs.
The team, from the Department of Anesthesia at Boston Children's Hospital, Harvard University, and the Massachusetts Institute of Technology, reported its results online on August 26 2012 in Nature Materials.
One of the major challenges in developing bioengineered tissues is creating systems to sense what is going on (eg chemically and electrically) within a tissue after it has been grown and/or implanted. Similarly, researchers have struggled to develop methods to directly stimulate engineered tissues and measure cellular reactions.
"In the body, the autonomic nervous system keeps track of pH, chemistry, oxygen and other factors, and triggers responses as needed," Daniel Kohane of Boston Children's Hospital explained. "We need to be able to mimic the kind of intrinsic feedback loops the body has evolved in order to maintain fine control at the cellular and tissue level."
The team built mesh-like networks of nanoscale silicon wires — about 80 nm in diameter — shaped like flat planes or in a "cotton-candy" like reticular conformation. The networks were porous enough to allow seeding with cells and encourage those cells to grow in 3D cultures.
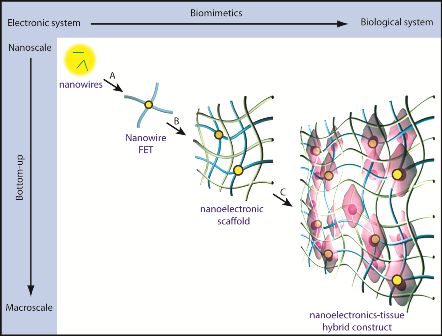
Figure 1. A schematic for integrating nanoelectronics with
engineered tissue, building 3D structures from nanowires and
transistors.
Source: Dr Bozhi Tian, Boston Children's Hospital.
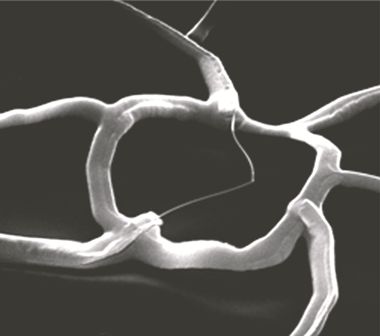
Figure 2. A single nanowire (at center) within its scaffolding.
Source: Dr Bozhi Tian, Boston Children's Hospital.
"Previous efforts to create bioengineered sensing networks have focused on 2D layouts, where culture cells grow on top of electronic components, or on conformal layouts where probes are placed on tissue surfaces," said Dr Bozhi Tian, also of Boston Children's Hospital. "It is desirable to have an accurate picture of cellular behavior within the 3D structure of a tissue, and it is also important to have nanoscale probes to avoid disruption of either cellular or tissue architecture."
"The current methods we have for monitoring or interacting with living systems are limited," said Charles Lieber of Harvard University. "We can use electrodes to measure activity in cells or tissue, but that damages them. With this technology, for the first time, we can work at the same scale as the unit of biological system without interrupting it. Ultimately, this is about merging tissue with electronics in a way that it becomes difficult to determine where the tissue ends and the electronics begin."
"Thus far, this is the closest we've come to incorporating into engineered tissues electronic components near the size of structures of the extracellular matrix that surrounds cells within tissues," Kohane added.
Using heart and nerve cells as their source material and a selection of biocompatible coatings, the team successfully engineered tissues containing embedded nanoscale networks without affecting the cells' viability or activity. Via the networks, the researchers could detect electrical signals generated by cells deep within the engineered tissues, as well as measure changes in those signals in response to cardio- or neurostimulating drugs.
Lastly, the team demonstrated that they could construct bioengineered blood vessels with embedded networks and use those networks to measure pH changes within and outside the vessels — as would be seen in response to inflammation, ischemia and other biochemical or cellular environments.
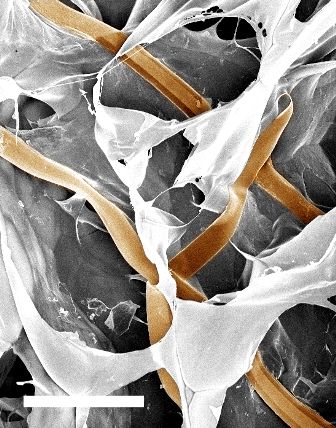
Figure 3. A nanoelectronic scaffold.
Source:
Dr Bozhi Tian, Boston Children's Hospital.
"This technology could turn some basic principles of bioengineering on their head," Kohane said. "Most of the time, for instance, your goal is to create scaffolds on which to grow tissues and then have those scaffolds degrade and dissolve away. Here, the scaffold stays, and actually plays an active role."
The team members see multiple future applications for this technology, from hybrid bioengineered "cyborg" tissues that sense changes within the body and trigger responses (eg drug release, electrical stimulation) from other implanted therapeutic or diagnostic devices, to development of "lab-on-a-chip" systems that would use engineered tissues for screening of drug libraries.