Stanford Hospital opens hybrid operating and angiography room
12 July 2010
Stanford Hospital & Clinics in California has developed a hybrid room where a patient can stay in one place to be diagnosed and treated, either with surgery or the latest interventional procedure, in an environment as sterile as an operating room, with all-important imaging devices, microscopes and monitors right at hand.
“It’s a quantum leap up,” said Robert Dodd, MD, PhD, who is both Stanford neurosurgeon and interventional neuroradiologist. “We can have a full operating team in the room and we won’t have to move the entire team and patient down the hall, up the elevator and back down again.”
The patient, in that old scenario, remains anaesthetized, and movement requires all the IV poles to come, too, along with a medical team. It also means that the surgical opening remains unclosed until imaging can confirm that the surgery has done what was needed. That kind of back and forth, Dodd said, can take all day, instead of four hours and no moving necessary.
“It’s much safer for the patient,” said Shelly Reynolds, RN, Interim Director of the Hospital’s Cath-Angio Interventional Services Lab. “If someone has their brain exposed, it’s not really ideal to be moving them down the hallway.” Until Room 9 opened, however, that was the only option.
Room 9, open only a couple of weeks, was designed specifically to allow on-scene collaboration between specialists in neurosurgery and neuroradiology. The room’s centerpiece is a stereoscopic biplane digital subtraction angiography system — its curvilinear arms nearly reaching the ceiling, encircling a space as broad as a giant redwood trunk. It’s a machine that captures all-around images of the brain without having to turn the patient from side to side. Because fewer images are required to build the 3D images that offer the required precision of detail, the patient is exposed to less radiation and less contrast dye injection.
The improved detail enhances patient safety as well as diagnosis and treatment. “Combined with live fluoroscopy, the newer angiographic hardware and software in the room produces a fully-dimensional image that reconstructs a patient’s arterial system,” said Michael Marks, MD, Chief, Interventional Neuroradiology. “We can understand anatomy better and more precisely navigate.”
The larger space is not just about the equipment, Reynolds said. In the older rooms, “people are literally up against the wall−attending physicians, anaesthesiologist, residents, nurses, technicians. It’s a lot of people in a very tight space. And that’s just essential personnel.”
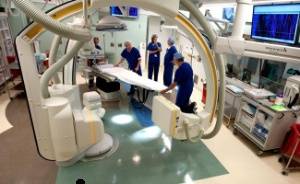
Stanford's hybrid room
Thirty years ago, the industry standard size for operating rooms was 450 square feet. Advanced imaging technology is now part of the standard equipment at top-flight hospitals, like Stanford, and that equipment requires space. The new industry standard operating room is at minimum, 600 square feet. New operating rooms must also accommodate the greater degree of collaboration between specialists that means more personnel around a patient. At 800 square feet, hybrid rooms like Stanford’s can hold those extra people that might be needed in an unanticipated turn of events, if what begins as a catheterization suddenly becomes a situation for surgery.
Neurocatheterization is a treatment option whose capabilities have grown rapidly in the last decade. In a typical procedure, Dodd will make a fingernail-sized opening at the top of a patient’s thigh and then thread a very tiny tube − the catheter − into an artery that will, ultimately, reach the patient’s brain. Once there, Dodd manipulates tools carried by the catheter to remove stroke-causing blood clots with exquisite specificity. It’s a procedure that requires the highest degree of imaging and must be done as precisely as any surgery, and yet, until now, hospital design has separated catheter procedures from operating rooms.
Planning Room 9 took months of careful evaluation of the needs of physicians, nurses and technologists, Marks said. The transformation was precipitated by the natural end of Room 9’s usefulness, said the Hospital’s Vice President-Clinical Services Jerry Maki. “We were convinced that a new hybrid room was what was needed at Stanford, so it made sense to invest the effort and funds to make it happen.”
The new Stanford Hospital will include one entire floor of this kind of multipurpose space, with several 1,000-square-foot units large enough to accommodate larger scale equipment and more people. In the meantime, the hospital is considering renovations, to surgical standards, of other catheterization procedure or operating rooms. Room 9 will not be restricted to neurological procedures. Many other fields of medicine — such as cardiology, vascular, thoracic, gastrointestinal — now include minimally invasive procedures guided by advanced imaging.