New PET imaging chemical gives 3-D image of immune response in action
29 June 2008
A new molecular probe developed at the University of California, Los Angeles (UCLA) Jonsson Comprehensive Cancer Center enables scientists to monitor the immune system at the whole body level in 3D, as it tries to fight some cancers or when it goes awry as it does in autoimmune diseases. The advance will allow scientists to model and measure the immune system in action and monitor response to new therapies.
The discovery, published June 8, 2008 in the early online edition of the journal Nature Medicine.
 |
|
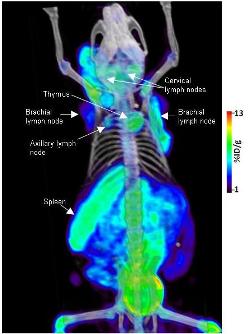
Autoimmune syndrome visualised
|
The researchers obtained the molecular probe, by modifying a common chemotherapy drug to create a new probe for Positron Emission Tomography (PET). Researchers created the small molecule, called FAC, by slightly altering the molecular structure of one of the most commonly used chemotherapy drugs, gemcitabine. They then added a radiolabel so the cells that take in the probe can be seen during PET scanning.
The probe is based on a fundamental cell biochemical pathway called the DNA Salvage Pathway, which acts as a sort of recycling mechanism that helps with DNA replication and repair. All cells use this biochemical pathway to different degrees.
But in lymphocytes and macrophages, the cells of the immune system that initiate immune response, the pathway is activated at very high levels. Because of that, the probe accumulates at high levels in those cells, said Dr. Owen Witte, a researcher at UCLA’s Jonsson Cancer Center, a Howard Hughes Medical Institute investigator and senior author of the study.
“This is not a cure or a new treatment, but it will help us to more effectively model and measure the immune system,” said Witte, who also serves as director of the Eli and Edythe Broad Center of Regenerative Medicine and Stem Cell Research at UCLA. “Monitoring immune function using molecular imaging could significantly impact the diagnosis and treatment evaluation of immunological disorders, as well as evaluating whether certain therapies are effective.”
Because the probe is labeled with positron emitting particles, cells that take it in glow 'hot” under PET scanning, which operates as a molecular camera that enables visualization of biological processes in living organisms. The work, done in animal models, will be further evaluated in subsequent studies. Eventually, Witte said, researchers hope to be able to monitor the immune systems of patients with FAC and other PET probes.
“This measurement is not invasive — it involves a simple injection of the probe,” Witte said. “We could do repetitive scans in a single week to monitor immune response.”
Using conventional methods, oncologists are forced to wait weeks and often months to determine whether a patient is responding to a therapy. CT and MRI scans are taken before and during treatment and the size of the tumour is measured to determine response — if the tumour is shrinking, the patient is responding. However, patients that don’t respond are exposed to potentially toxic therapies for longer than necessary. If the new PET probe can monitor immune response and response to treatment much more quickly — within a week or two — patients would be spared from therapies that aren’t working.
One frustrating aspect for many cancer researchers is understanding the role of the immune response in fighting or, in some cases, possibly stimulating tumour growth, said Dr Kevin Shannon, the Auerback Distinguished Professor of Molecular Oncology at the University of California, San Francisco.
“Dynamic probes like the one developed by UCLA scientists will allow researchers to learn more about the role of the immune response in cancer, how current treatments affect immune cells, and will allow them to quantitatively monitor responses to new modalities such as tumour vaccines,” Shannon said. “Probes of this type may also help oncologists more rapidly identify tumours that will respond to certain drugs so treatments can be made more patient-specific.”
Witte said the type of multidisciplinary research that led to development of the probe is uniquely suited to UCLA’s collaborative strengths. Researchers from the cancer center, the Broad stem cell center and the Crump Institute for Molecular Imaging took part in the study. The PET scanner was invented by UCLA’s Michael Phelps, also a co-author on this study.
The work by Witte and his colleagues was prompted by the desire to add to a short list of probes now used in PET scanning and to develop new probes that monitor different molecular functions than the current probes.
“What we wanted to do was to develop new ways to look inside a living organism and gather as much information as we can about the immune system,” said Caius Radu, an assistant professor of molecular and medical pharmacology, a Jonsson Cancer Center researcher and the first author of the study. “We wanted to know how cells move from one site in the body to another and find a way to trace them to tumours.”
In previous studies, Witte and other UCLA researchers were able to track the immune system as it recognized and responded to cancer. But in those studies, the cells had to be modified with 'reporter' genes that sequestered a specifically designed PET probe that allowed scientists to monitor them.
The new probe doesn’t require modified cells, making it easier and less expensive to use and giving it far broader applications than existing probes. In addition to modeling and measuring the immune system, those applications include stratifying different types of cancers and their response to therapy, defining the level of immune response in both normal and pathological situations and helping to determine whether new drugs prompt an immune response to cancer and other diseases.
“This probe will tell us things about the immune system that existing probes can’t,” said Radu, who also is a member of the Crump Institute for Molecular Imaging.